November 14, 2025

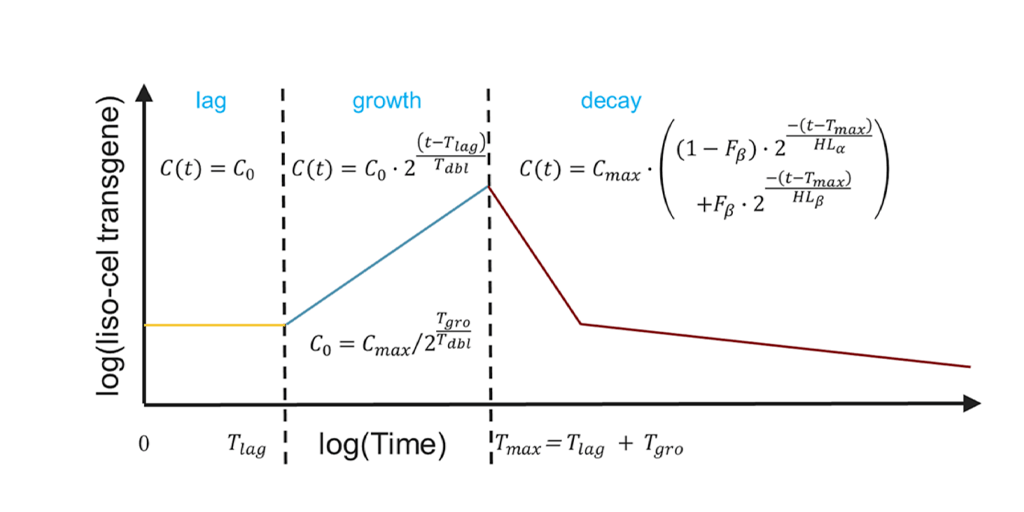
Capturing CAR T-cell Therapy Dynamics Through Mechanistic Modeling
Watch our on-demand webinar to learn more about Capturing CAR T-cell Therapy Dynamics Through Mechanistic Modeling

Senior Director, Clinical Pharmacology and Translational Medicine
Dr. Osborn has over 25 years of drug development experience in the areas of clinical pharmacology and pharmacokinetics. She has focused primarily oncology and anti-infectives. Before joining Certara, she was a reviewer in the Office of Clinical Pharmacology, US Food and Drug Administration, in the Division of Cancer Pharmacology, CDER where, she participated in the assessment of multiple dose justification submissions under Project Optimus. Prior to working in the FDA, she was a clinical pharmacologist in the National Institute of Allergy and Infectious Diseases (NIAID) at the National Institute of Health (NIH). There, projects were focused on therapeutics and vaccines in the infectious disease area. She worked on design and support of phase 1 trials, bioanalytical assay development and validation, and projects using the “Animal Rule” to support development of countermeasures in situations where clinical trials were not ethical or feasible. Dr. Osborn has held roles supporting both clinical and nonclinical pharmacology drug development for large molecules in biotechnology companies including Human Genome Sciences and CoGenesys. She is particularly interested in early phase drug development, including dose selection and justification strategies to speed development of therapeutics.
Dr. Osborn is holds a Ph.D. in Pharmacology from The George Washington University and is based in the Washington DC metropolitan area.

Content Marketing Manager
Charlotte is a content marketing specialist with ten years’ experience planning and executing corporate marketing strategies. She works within Certara’s Content Marketing team, developing educational and persuasive content primarily supporting the Pinnacle 21 platform. Charlotte joined the Certara team during the acquisition of Formedix in 2023.
References
[1] Bullock JM, Lin T, & Bilic S. (2017). Clinical pharmacology tools and evaluations to facilitate comprehensive dose finding in oncology: A continuous risk-benefit approach. J. Clin. Pharmacol., 57(510), 5105–5115.
[2] Ishida Y, Murai K, Yamaguchi K, et.al. (2016). Pharmacodynamics and pharmacodynamics of dasatinib in the chronic phase of newly diagnosed chronic myeloid leukemia. Eur. J. Clin. Pharmacol., 72(2), 185–193.
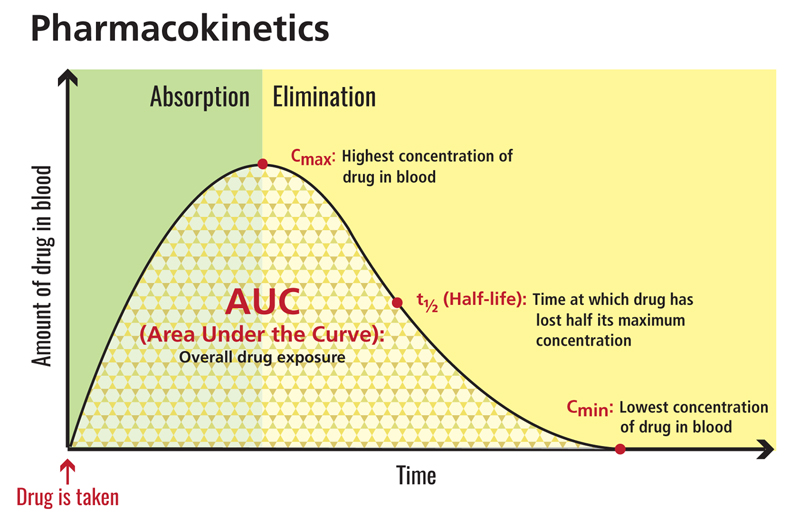
[4] clinicalinfo.hiv.gov. (n.d.). Area Under the Curve (AUC) | NIH. [online] Available at: https://clinicalinfo.hiv.gov/en/glossary/area-under-curve-auc.
[3] US Department of Health and Human Services, Food and Drug Administration, Center for Drug Evaluation and Research. (2016). Clinical Pharmacology Review, Application Number 205552Orig1s000. Retrieved from https://www.accessdata.fda.gov/drugsatfda_docs/nda/2013/205552Orig1s000ClinPharmR.pdf
This blog was originally published in April 2018, and has been updated for accuracy.
Learn more about Modeling and Simulation Services
Certara’s modeling and simulation services provide valuable insights, de-risk your projects, optimize decisions, and accelerate timelines across all phases of drug development.

Contact us