March 19, 2026
Permanent shift to hybrid work
A 2023 survey of healthcare decision-makers found a solid transition to hybrid or remote work environments since the pandemic. Their use of digital resources either stayed the same or increased; it never went back down.
These decision-makers now spend more than twice as much time reviewing digital vs. non-digital materials [3].
Increase in product complexity
The rise of specialty medicines, cell and gene therapies, and precision oncology means that value conversations require nuanced, data-rich engagement.
Discussions must demonstrate clinical differentiation, budget impact, and outcomes evidence tailored to specific patient populations and care-settings
Diversification of the payer environment
The stakeholder universe now includes pharmacy benefit managers, integrated delivery networks, health systems with payer functions, clinical pathway organizations, and government agencies.
Each has distinct information needs, decision criteria, and engagement preferences [4][5].
- Increasing regulatory and payer pressure
- Payers are tightening cost-effectiveness expectations
- The nature of new medicines is changing
- Value stories must address complex evidence challenges
New drug approvals with orphan designations
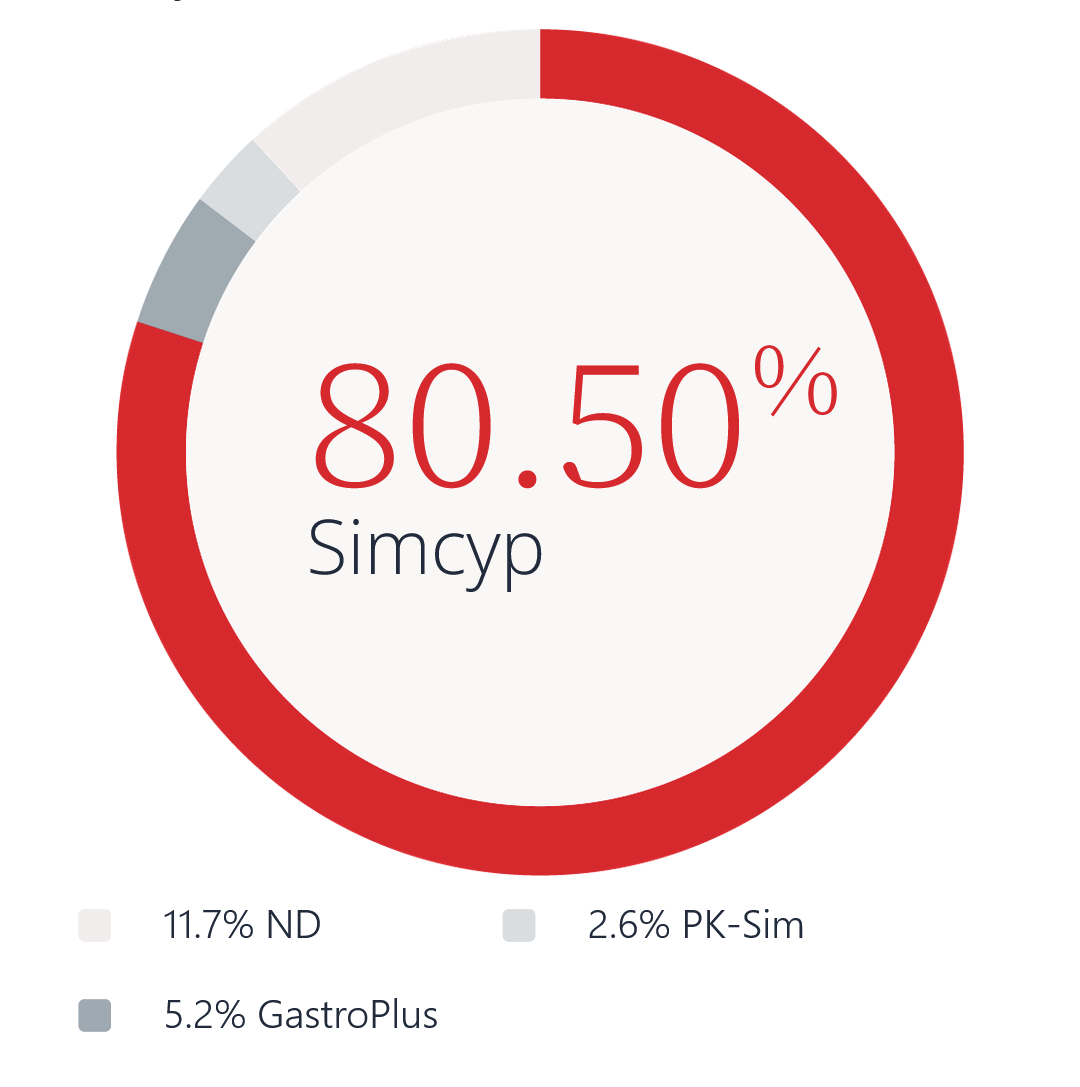
US launches comprising specialty medicines
- Live modeling powers the experience
- Evidence and analysis live in a single environment
- Payers become active participants in live analysis
- Analytics reveal what shapes payer decisions
- Regulatory compliance is embedded in the platform

Ready to boost payer persuasion?
Explore an alternative to static spreadsheets and slides – see the value story in action with the BaseCase demo app. You’ll see how BaseCase turns your value strategy into interactive tools that field teams can use to persuade payers and decision makers.
References and notes
1. QVIA Digital Innovation Summit; IQVIA Institute data, 2024–2025.
2. eMarketer, “U.S. Healthcare and Pharma Ad Spending 2024.”
3. AmerisourceBergen, “Assessing the Evolving Landscape of Digital Engagement Between Healthcare Decision Makers and Biopharma Companies,” 2023.
4. PharmExec, “Biopharma Market Access: The Pivot to Payer Omnichannel Engagement,” 2025.
5. PharmExec, “Integrating Payers Into Your Digital Communication Plan.”
6. ZS, “Pharmaceutical Industry Trends 2025: Outlook and Strategies.”
7. TRiBECA Knowledge, “Market Access 2025: Navigating HTA and Drug Reimbursement Challenges.”
8. Simon-Kucher, “From AI to LMICs: Four Global and Regional Trends Impacting Pharma P&MA,” 2025.
9. Cencora, “FormularyDecisions Enterprise Biopharma-Payer Engagement.”
10. Clarivate/DRG Digital, “Multichannel Payer Marketing Study.”
11. Fierce Pharma, “Advice for Pharma Involved in Payer Marketing: Ramp Up Digital.”
12. Cencora, “Empowering Healthcare Decision-Making: FormularyDecisions Five-Year Reflection.”
This blog was originally published on July 29, 2022 and has been updated for accuracy.

Christian Pichardo
Director, Product ManagementChristian Pichardo serves as Director of Product Management at Certara/BaseCase. He leads the design and strategic direction of digital solutions that strengthen health economics and value communication, ensuring alignment with customer needs and market trends.
Before stepping into his current role, Mr. Pichardo spent more than 15 years working across the life sciences, consulting, and software industries, holding leadership roles in market access, health economics, and product strategy. In addition to his corporate experience, he has co-founded consulting ventures focused on healthcare innovation and capability development, further broadening his perspective on advancing access and value in healthcare.
Mr. Pichardo holds degrees in Economics and Applied Mathematics from the Instituto Tecnológico Autónomo de México (ITAM) and a Professional Certificate in Product Management from the Massachusetts Institute of Technology (MIT). He has published peer-reviewed research on cost-effectiveness and real-world outcomes in leading scientific journals.
Make an inquiry
Ready to bring your value story to life? Make an inquiry to learn how BaseCase value communication software transforms complex economic models and clinical data into interactive, field-ready tools.
FAQs
What is payer engagement in pharma?
Payer engagement in pharma refers to how pharmaceutical organizations communicate the clinical, economic, and real-world value of therapies to those responsible for reimbursement decisions. These stakeholders include insurers, pharmacy benefit managers, and health system providers.
Effective payer engagement strategies ensure decision-makers can assess clinical outcomes, cost-effectiveness, and budget impact when determining formulary placement and coverage policies.
What payer engagement strategies are most effective for pharmaceutical companies?
Successful payer engagement strategies combine scientific evidence, economic modeling, and personalized messaging tailored to each payer’s decision environment. Leading pharma teams use a mix of field engagement, early value communication, and pharma digital engagement platforms that allow payers to explore data interactively. This approach helps stakeholders understand clinical differentiation and financial impact in the context of their own patient populations.
What tools are available for managing pharmaceutical payer engagement?
Modern payer engagement tools help pharmaceutical teams deliver complex evidence in a more interactive and analytical format. The most advanced solutions function like a payer engagement app, allowing payers to explore clinical data, run budget impact models, and evaluate coverage scenarios using their own assumptions.
How does pharma digital engagement improve payer communication?
Pharma digital engagement enhances payer communication by replacing static presentations with interactive experiences. Digital platforms allow payers to adjust economic model inputs, explore treatment scenarios, and review clinical evidence in real-time. This form of payer engagement in pharma enables a more collaborative discussion where stakeholders actively analyze data, rather than passively receiving information.
What is a payer engagement app and how is it used in pharma?
A payer engagement app is a digital platform designed to support communication between pharmaceutical companies and payer organizations. These apps integrate clinical evidence, health economic models, and payer-specific data into a single environment. As part of broader payer engagement strategies, they allow account teams and decision-makers to explore treatment value, simulate budget impact, and review evidence together in live discussions.